• Male Suspensory
For the Nigerian man who wishes to take the burden of family planning off his wife, the condom and vasectomy, a surgical procedure to cut the vas deferens, the tubes that carry a man’s sperm from his scrotum to testicles remain the only available contraceptive options. Unfortunately, most men have found the two methods unsuitable for their family planning needs. For instance a study showed that 85% sexually active men in the country don’t use the condom while only 30% of married men who patronise prostitutes bother to use it. A study published by the Ghana Medical journal recently reported that even a large number of Nigeria’s doctors are not favourably disposed to vasectomy as a contraceptive.
But if various research findings around the world is anything to go by, the trend may soon change as men will soon have different contraceptive options to choose from in their quest to have only the number of children they can adequately cater for. Although several of these contraceptives are close to market, none are currently available. Some methods are still in basic science stages, some have been tested in animals only, while some have entered the process of clinical trials required for government approval.
This array of devises should be of interest to most men. Like the female methods they offer a wide variety of choice for the modern men. They include the Heat method, injectables hormonal methods among several others. Here are some of the latest devices as published recently by malecontraceptives.org.
Suspensories/Internal heat
Suspensories are specially designed briefs that hold the testes closer to the body, raising their temperature. The development of the male suspensory is premised on the well known theory that a small increase in the temperature of the testes has a large negative impact on the production of sperm (spermatogenesis). A team of researchers in France have carried out clinical trials of various suspensory designs as male contraceptives Their results showed that men who wore one suspensory design with a rubber ring to hold the testes in the inguinal canals had 100% effective contraception. All trial participants achieved very low motile sperm counts, between 0 and 1.6 million sperm per milliliter. Because the change in temperature is only a few degrees, suspensories must be worn daily to provide effective contraception. Clinical trials show that suspensories can suppress sperm counts and make the remaining sperm poor swimmers.
There are many different suspensory designs, but generally they look from the outside like a normal pair of brief underwear or an athletic support. Some suspensory designs leave the scrotum and penis free. All designs hold the testes inside the lower ends of the inguinal canals. Suspensories must be worn every day during waking hours to be effective.
Tests of suspensories have all shown full recovery to pre-treatment sperm count and motility levels. The length of time to recovery depends on the duration of the treatment. In a 1 year trial, men returned to pre-treatment levels within 12-18 months. However, full recovery is not necessary to achieve a pregnancy; one man fathered a child 3 months after stopping treatment
RISUG
RISUG, an acronym for Reversible Inhibition of Sperm Under Guidance, is an injectable compound that partially blocks the vas deferen (tubes that carry sperm), providing effective contraception for up to 10 years per dose. It is effective immediately, has few side effects, and has proven to be reversible in primate studies. This contraceptive has completed Phase I and II clinical trials in India
RISUG has two contraceptive effects: partial blockage of the vasa deferentia and disruption of the sperm that pass through it. The men who participated in that first trial have had RISUG implanted for 15 years and counting with no complications.
The Phase II clinical trial volunteers have now been using RISUG for more than ten
years. Primate studies have shown that RISUG is readily reversible, but reversal has not yet been tested officially in humans. Researchers say since RISUG does not cause the type of auto-immune response associated with vasectomy, RISUG reversal should be much more reliably successful.
Injected plugs
Injected plugs were developed in China as a potential alternative to vasectomy. The concept is similar to the Intra Vas Device, except that instead of implanting pre-formed plugs, the plugs are injected into the vasa deferentia in liquid form. The plugs then harden in place and block the flow of sperm. Two different types of injected plugs have been tested: medical-grade polyurethane (MPU) and medical-grade silicone rubber (MSR). Starting in the early 1980s, thousands of Chinese men chose MPU plugs as an alternative to vasectomy. Estimates of the number of men with plugs range from 13,500 to 300,000 (Zhao 1992b).
Intra Vas Device (IVD)
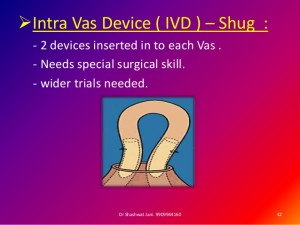
The Intra Vas Device (IVD) is a set of tiny implants that block the flow of sperm. There are two IVD designs in clinical trials. One is a pair of soft, silicone plugs made by the Shepherd Medical Company in the United States. The other is a urethane tube lined with a tiny nylon sieve made by the Foshan Medical Company in China. Both of these designs were inspired by the 1980s work of Dr. Lourens Zaneveld, who showed in pilot studies that the IVD is a safe and effective method of male contraception.
Because the materials used in both IVD designs have been widely tested and shown safe for medical use, researchers hope that these IVDs will encounter few regulatory hurdles. When the US design hits the market, Shepherd Medical predicts that the combined cost of the device and the insertion procedure will be under $1,000.
External heat
This is similar to Suspensories as it subjects the testes to heat to ensure sperm counts drop. Because an external heat source can be significantly warmer than body temperature, the duration of exposure required for effective contraception is shorter than for suspensories.
Optimal sperm production (spermatogenesis) requires temperatures several degrees Celsius below average body temperature. The testes are located outside the body in the scrotum, which has several mechanisms to keep the testes cooler than the rest of the body. Warming the testes to or above body temperature temporarily disrupts spermatogenesis
The main evidence for effective use of external heat as a male contraceptive comes from the unpublished works of a Swiss doctor working in India between 1930 and 1950. Dr. Martha Vogeli advised 100s of men on the use of hot sitz baths, and claims that her patients attained 100% effective contraception using this method . Dr. Vogeli tested baths in a range of temperatures with 9 volunteers to determine the most effective regimen. She determined that 21 consecutive days of 46.5 ºC (116 ºF) sitz baths lasting 45 minutes typically provided 6 months of contraception. As a high-tech and perhaps more convenient alternative to hot sitz baths, several inventors have created batterypowered pouches designed specifically to heat the testes.
Male hormonal contraceptives
Commonly known as the “male pill”, a hormonal contraceptive for men will probably not be delivered as a pill. Researchers are coming closer to a marketable male hormonal contraceptive (MHC) delivered by injection or implant, but there is nothing commercially available right now. Researchers have found several effective formulations and delivery methods – shots, implants, gels and pills. Several MHC formulations are as effective and safe as the female birth control pill.
Male hormonal contraceptives attempt to block or severely reduce the production of sperm. They accomplish this by stopping the secretion of a man’s reproductive hormones in the brain and testes. When levels of testosterone in the testes are low, sperm production slows or halts.
The ultimate goal of all MHC methods is azoospermia, or the complete absence of sperm in the ejaculate. Researchers agree that severely oligospermic men with fewer than 1 million sperm per milliliter of semen are functionally infertile.
Adjudin
Adjudin is a new drug and an analogue of an old drug known as lonidamine. Lonidamine is an anti-cancer medication whose contraceptive effect was discovered in the 1980s. Researchers did not pursue lonidamine as a male contraceptive because at high doses it caused kidney damage. Since then, a group of scientists at New York’s Population Council, a nonprofit contraceptive research organization, have sought compounds less toxic than, but functionally similar to, lonidamine. Advances in screening technology led to the identification of several promising nontoxic compounds in the late 1990s. One of these compounds – AF-2364 or Adjudin – is moving toward trials in humans.
Adjudin provides contraception by disrupting the process of sperm maturation in the testes. It changes the way Sertoli cells – which divide to produce new sperm cells and then nurse the immature sperm – interact with sperm. In normal sperm production, Sertoli cells remain connected with immature sperm through a series of microscopic bridges and channels. These bridges provide materials and information needed to direct the development of the immature sperm (spermatids).
‘Dry orgasm’ pill
This was reported by a Nigerian Dr. Nnaemeka Amobi and his British colleague Dr. Christopher Smith 2006. They were reported to have been working since 1995 to discover how two drugs – phenoxybenzamine, a high blood pressure medication, and thioridazine, a discontinued schizophrenia medication – each act as a male contraceptive. As early as the 1950s, doctors with patients taking these drugs to regulate their blood pressure and mental health noticed that their patients became infertile. It turns out that the two drugs have a similar contraceptive effect.
During sexual arousal, some of the sperm in the epididymis are propelled by smooth muscle contractions along the vas deferens (plural: vasa deferentia). When the vasa deferentia meet the urethra, the sperm mix with fluids made by the seminal vesicle and prostate, forming semen. Finally, during orgasm the semen is propelled through the urethra by more smooth muscle contractions and ejaculated. The smooth muscles in the male reproductive system are not under conscious control; they contract and relax according to signals from the autonomic nervous system.
